To link to this article from your blog or webpage, copy and paste the url below into your blog or homepage.
The Mental Health Care System
an article by our site
In urban America, living in subway tunnels, on steam grates, and in cardboard boxes we find more and more deinstitutionalized mentally ill. Why are the mentally ill on the streets?

This mentally ill unfortunate is bouncing off the walls in a padded cell designed to keep him from hurting himself
First, some background: The type of care we have provided the mentally ill has gone through numerous shifts over the years—motivated politically, economically, and more rarely, morally.
During colonial and federalist periods, psychotic and other dependent persons were "cared for" by local communities. Almshouses and jails were overrun with mentally ill who were often treated more cruelly than the criminals.
After the Civil War, with funding reduced, these hospitals gave up active treatment and turned into enormous holding units. The ill were often treated brutally, and, at best, were treated with indifference, save their needs for shelter and food. This went on until after World War II at which time there were over 500,000 patients in these institutions (accounting for over half of all the hospital beds in the country).
Then, in the second quarter of the 19th century a group began what they called "moral" care, believing that if treated right, given good models, encouraged to establish order in their lives, the mentally ill might recover. Dorothea Dix's efforts across the country to this end resulted in a network of state-operated hospitals where doctors often discharged their patients within a year.
At this point in time a new generation of psychiatrists returning from the war began emphasizing the desirability of preparing patients to return to the community. Reforms in the state systems began. This, along with the discovery and use of Thorazine in 1952, which controlled the symptoms of psychosis, fueled the new psychiatric enthusiasm for community-based care. From a high of 558,922 patients in 1955, the number decreased gradually to 475,000 in 1965.
Then, suddenly there were many proponents of community care declaring that all treatment should take place in the community. The belief was that the institutions caring for the mentally ill, by their own nature, fostered the symptoms they were trying to treat. So in 1963, the Community Mental Health Center Act was born, which provided seed money from the federal government to develop 2000 outpatient clinics in every area of the country. Then the civil-libertarian attorneys started crusading for the autonomy of the mentally ill and eventually, through the judicial process, states forbid involuntary commitment except for those who were defined as dangerous to themselves or others. It was also supposed that community care would cut expenses.

At first psychiatrists determining the fate of the patients—later it became a judicial and political process
And the movement which had begun gradually with the psychiatrists determining the fate of the patients, continued as a judicial and political process: patients were to be released at all cost; new admissions were discouraged. But at the same time, less than half of the 2000 centers were built. And of those that were built, many lost their funding and had to turn to more desirable patients, those less disturbed, and those insured or able to pay. I.e., the craziest and most dangerous ended up on the street.
By 1975 state hospitalization dropped to 193,000. By 1980, the number was 137,000 (Appelbaum, Paul S., "Crazy in the Streets, The Policy of Deinstitutionalization," Currents, October 1987, pp. 4-10), and in 1984, 114,000. (Hop, Marjorie, and Young, James, "Who Cares For the Mentally Ill?" The Nation, December 26, 1987/January 2, 1988, pp. 782-784) However, very few state hospitals closed. (Statistical Abstract of the U.S., 1988, 108th ed) Instead of caring for thousands of patients, they care for a few hundred. As many hospitals existed in 1980 as in 1955, with less than one quarter of the patients. As care is less and less available, state mental-health budgets continue to expand (Source: Appelbaum, Paul S., "Crazy in the Streets, The Policy of Deinstitutionalization.") with hospitals receiving 70 percent of public funds allocated for mental health, while there are 16 times the patients in outpatient facilities. (Hop, Marjorie, and Young, James, "Who Cares For the Mentally Ill?")

A hospital ward
So where are the patients? It is estimated that 750,000 live in nursing homes or in board and care homes, many of which have locked wards just like the old state hospitals. And the rest live on the street. Depending on which study you read, between 40 and 60 percent of homeless persons are mentally ill.
There are lots of different national estimates of the extent of U.S. homelessness. None of these estimates are the last word on "how many people are homeless.” In a recent approximation USA Today estimated 1.6 million people used transitional housing or emergency shelters and 1/3 are members of households with children, a nine percent increase since 2007. Another approximation is from a study done by the National Law Center on Homelessness and Poverty which states that approximately 3.5 million people, 1.35 million of which are children, are likely to experience homelessness in a given year (Source: National Law Center on Homelessness and Poverty, 2007).
"The irony of the reforms is that by our belief in the autonomy and freedom of the mentally ill, we have caused their oppression. We have disguised as their liberty our failure to recognize the needs of thousands of mentally ill. We have abdicated our responsibility to do good for our fellow man. And though we might deprive him of his autonomy in the short run by committing him to an institution and providing treatment, in the long run he has a chance at true autonomy. Our current system provides him no chance at all." (Source: Appelbaum, Paul S., "Crazy in the Streets, The Policy of Deinstitutionalization.")
Others also believe than no long-term plan of community services can keep all patients out of hospitals. There is a cry for more money while cities, states, and the federal government play "chicken" to see which will shoulder the financial burden of the mentally ill. In all the squabbling, nothing is done. Emergency room personnel negotiate with private hospitals and nursing homes who have quotas and rules to keep patients out. These patients are ultimately sent to overcrowded wards of city hospitals, the dumping grounds for patients no one else will take. (Source: Goode, Erica E., "When Mental Illness Hits Home," U.S. News & World Report, April 24, 1989, pp. 55-65)

Medicaid pays for clinic services, but only if deemed medically necessary
"The mental health system is a crazy quilt of conflicting regulations and responsibilities. Medicaid will not pay for room and board in foster homes, halfway houses or group homes, although it may cover admission to hospitals or nursing homes. In most states it pays for clinic services, but only if deemed medically necessary. . . . State discretion is so broad that some states limit mental health clinic visits to eighteen per calendar year.
"In most places no agency at the state or local level takes responsibility for planning and implementing a system to assure that the mental health and community-support needs of the mentally ill will be met, or for monitoring the quality of institutional and community support programs. Nor does the N.I.M.H. assume leadership.
"Can we afford universal health care? The reality is that our privatized approach is the most expensive in the world." (Source: Hop, Marjorie, and Young, James, "Who Cares For the Mentally Ill?") But the "(un)Affordable Care Act," also known as Obama's Folly or ObamaDon'tCare, has just made things worse, in 2013-2014. Much worse—to the degree it will reverse the recovery from the Great Recession as it makes insurance companies richer than God. ObamaDon'tCare "accomplished" the following: People losing coverage all over the place, after being promised that no one would lose coverage and rates wouldn't increase, so now there is more people than ever without insurance and rates did go up. He promised people could keep their current policy, yet his Folly created conditions whereby many of these current policies were cancelled—another prevarication.

Surveys are great marketing, sociological, and demographic research tools
A 1988 study (Source: National Institute of Mental Health, Archives of General Psychiatry, November 1988) concluded that about 1/3 of all Americans suffer from a mental illness at some point in their lives (based on an 8-year survey of 18,571 adults around the U.S.). The majority, if these estimates are correct, never seek treatment. Between 12 and 22 percent of American children suffer from some type of mental or emotional disorder—depression, hyperactivity, chronic drug use, anorexia, etc. Whether there is now more mental illness among children than in the past or whether diagnosis and reporting have improved is unknown. What is true is that kids aren't getting help they need from parents, schools or mental health professionals. Only about a third of kids suffering from a mental disorder receive professional treatment even though the ability to understand, prevent, and treat many mental diseases in youngsters has improved over the past 40 years. (Source: Louv, Richard, Childhood's Future, Boston: Houghton Mifflin Company, 1990, pp. 166-167) Even preschool children are being treated for depression, whereas it was argued in the 70s whether depression could be diagnosed in pre-adolescents and children. (Source: Osius, Isobel, "A Day Late & A Dollar Short," Marketing Tools Alert, September 1991, pp. 4, 6, 8, 16)

58 percent of depressed women telephone a friend, and 35 percent of depressed men watch TV, but many drink or do nothing
When people are depressed, women and men tend to respond differently, according to a survey by Roper Organization in 1988. While 58 percent of women telephone a friend, only 29 percent of men do this. The most likely thing a man does when depressed is watch TV (35 percent). (Source: "Bye Bye Blues," American Demographics, September 1989, p. 16)

When depressed, 58 percent of women telephone a friend
Mental patients were about nine times more likely to be arrested for rape, robbery, aggravated assault, and burglary than the general population of the county. (Source: Larry Sosowsky, Crime and Violence Among Mental Patients Reconsidered in View of the New Legal Relationship Between the State and the Mentally Ill, 135 Am. J. Psychiatry 33-42, 1978)

Road rage can be temporary insanity or a sociopath acting antisocial; one thing for sure—it's dangerous
At least half of mass murderers (as well as many other murderers) have histories of mental illness. Many have already come to the attention of the criminal justice or mental health systems before they become headlines. In the early 1980s, there were about two million chronically mentally ill people in the United States, with 93 percent living outside mental hospitals. The largest diagnosis for the chronically mentally ill is schizophrenia, which afflicts about 1 percent of the population, or about 1.5 percent of adult Americans. A 1991 estimate was that schizophrenia costs the United States about $65 billion annually in direct and indirect costs. (Source: R. J. Wyatt, I. Henter, M. C. Leary & E. Taylor, An Economic Evaluation of Schizophrenia-1991, 30 Soc. Psychiatry & Psychiatric Epidemiology 196-205)
If the chart below looks like school slayings are not increasing, look again at the dates. The last range is for 3 years, the others are for a decade. Going "postal" is increasing at an alarming rate.

Deinstitutionalization played a substantial role in the dramatic increase in violent crime rates in America in the 1970s and 1980s. People who might have been hospitalized in 1950 or 1960 when they first exhibited evidence of serious mental illness today remain at large until they commit a serious felony. The criminal justice system then usually sends these mentally ill offenders to prison, not a mental hospital. (Source: Madness, Deinstitutionalization & Murder, Clayton Cramer, The Federalist Society for Law and Public Policy Studies)
More recently: In 2011, there were an estimated 45.6 million adults aged 18 or older in the United States with any mental illness (AMI) in the past year. This represents 19.6 percent of all adults in this country. These estimates were stable between 2008 (44.0 million, 19.6 percent) and 2011.
Among adults aged 18 or older in 2011, 11.5 million (5.0 percent) had serious mental illness (SMI) in the past year. These estimates of adults with SMI in 2011 were higher than the estimates in 2008 (9.9 million, 4.4 percent), but were similar to those in 2009 (11.0 million, 4.8 percent) and 2010 (11.5 million, 5.0 percent).
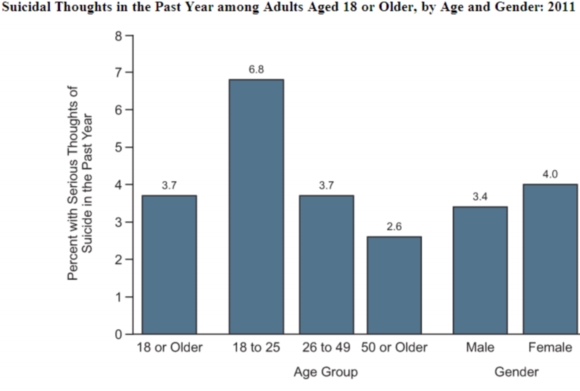
Women aged 18 or older were more likely than men aged 18 or older to have past year any mental illness (23.0 vs. 15.9 percent) and serious mental illness (6.4 vs. 3.4 percent) in 2011.

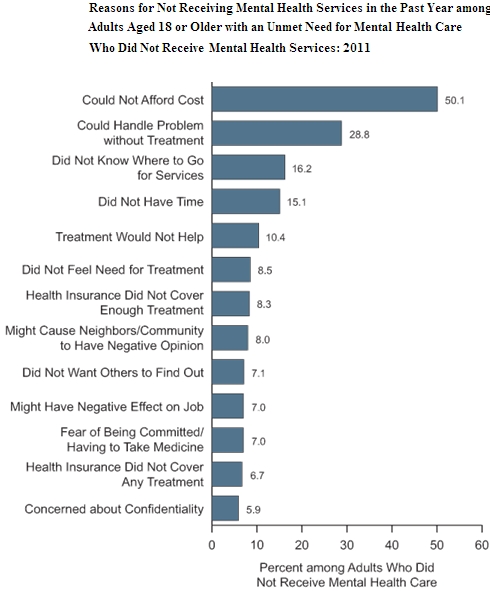
(Source for charts below: Results from the 2011 National Survey on Drug Use and Health: Mental Health Findings; Center for Behavioral Health Statistics and Quality (CBHSQ), Substance Abuse and Mental Health Services Administration (SAMHSA), U.S. Department of Health and Human Services (HHS), and by RTI International)


The bad news? Big Pharma is pushing shrinks to be drug pushers who define psychological issues as brain defects needing drugs.
The worse news? Many are buying into that nonsense!
See Reclaiming Our Children.

Breggin clearly demonstrates in Reclaiming Our Children that we aren’t actually a nation of crazies and defectives needing to be saturated in psychiatric pharmaceuticals to fix our broken brains





